Do Fallen Arches Involve Surgery?
Overview

Fallen arches are a condition of the feet that can cause pain and discomfort. Normally, you should see an arch in the bottom of your foot. That arch is created by the tendons in your feet. The tendons pull, which forms the arch. Sometimes, the tendons do not pull as they should, which results in the condition of fallen arches. If you have fallen arches, your feet may look flat. You might also notice when you see your bare footprint that the arch is not visible in the print. It is fairly common for children to have flat feet, but the arch usually develops as it should as they get older. For adults, fallen arches can be quite painful and problematic.
Causes
The most common acquired flat foot in adults is due to Posterior Tibial Tendon Dysfunction. This develops with repetitive stress on the main supporting tendon of the arch over a long period of time. As the body ages, ligaments and muscles can weaken, leaving the job of supporting the arch all to this tendon. The tendon cannot hold all the weight for long, and it gradually gives out, leading to a progressively lower arch. This form of flat foot is often accompanied by pain radiating behind the ankle, consistent with the course of the posterior tibial tendon. Compounding matters is the fact that the human foot was not originally designed to withstand the types of terrain and forces it is subjected to today. Nowhere in nature do you see the flat hard surfaces that we so commonly walk on in present times. Walking on this type of surface continuously puts unnatural stress on the arch. The fact that the average American is overweight does not help the arch much either-obesity is a leading cause of flat feet as the arch collapses under the excessive bodyweight. Furthermore, the average life span has increased dramatically in the last century, meaning that not only does the arch deal with heavy weight on hard flat ground, but also must now do so for longer periods of time. These are all reasons to take extra care of our feet now in order to prevent problems later.
Symptoms
Many people have flat feet and notice no problems and require no treatment. But others may experience the following symptoms, Feet tire easily, painful or achy feet, especially in the areas of the arches and heels, the inside bottom of your feet become swollen, foot movement, such as standing on your toes, is difficult, back and leg pain, If you notice any of these symptoms, it's time for a trip to the doctor.
Diagnosis
It is important for people with foot pain to know if they have flat feet. The following tests can help you determine your arch type. When you get out of a swimming pool, look at your footprint on the concrete. The front of the foot will be joined to the heel by a strip. If your foot is flat, then the strip is the same width as the front of the foot, creating a footprint that looks like a stretched out pancake. With a normal arch, the strip is about half the width of the front of the foot. If you have a high arch, only a thin strip connects the front of the foot with the heel. Put your shoes on a flat table and view them at eye level from behind. See if the sole is worn evenly. A flat foot will cause more wear on the inside of the sole, especially in the heel area. The shoe will easily rock side to side. A flat foot will also cause the upper part of the shoe to lean inward over the sole. Both shoes should wear about the same way. If you have pain in one foot, you should make sure you don't have a fallen arch on that side. There are two good tests you can perform at home to detect this problem. Place your fingertips on a wall that you are directly facing and stand on your tiptoes on one foot. If you can't do it, a fallen arch may be the culprit. Stand with your feet parallel. Have someone stand in back of you and look at your feet from behind. You can also do it yourself if you stand with your back to a mirror. Normally, only the pinky toe is visible from behind. If one foot is flatter than the other, the 4th and sometimes the 3rd toe on that foot can also be seen.
What does it mean when you have flat feet?
Non Surgical Treatment
Ligaments hold up arches. Deformed ligaments will not return to their original shape, just as an overstretched rubber band remains elongated. Arch supports help restore more normal function. Not all orthotics are made alike. Sole Supports custom designed orthotics are unique in the way they are cast. Sole Supports compensate for the differences between each foot. They take into account your body weight and the degree of flexibility in your feet. Taking care of fallen arches can be key in dealing with unresolved or recurrent back pain.
Surgical Treatment

Surgery for flat feet is separated into three kinds: soft tissue procedures, bone cuts, and bone fusions. Depending on the severity of the flat foot, a person?s age, and whether or not the foot is stiff determines just how the foot can be fixed. In most cases a combination of procedures are performed. With flexible flat feet, surgery is geared at maintaining the motion of the foot and recreating the arch. Commonly this may involve tendon repairs along the inside of the foot to reinforce the main tendon that lifts the arch. When the bone collapse is significant, bone procedures are included to physically rebuild the arch, and realign the heel. The presence of bunions with flat feet is often contributing to the collapse and in most situations requires correction. With rigid flat feet, surgery is focused on restoring the shape of the foot through procedures that eliminate motion. In this case, motion does not exist pre-operatively, so realigning the foot is of utmost importance. The exception, are rigid flat feet due to tarsal coalition (fused segment of bone) in the back of the foot where freeing the blockage can restore function.
Prevention
Flat feet or Fallen Arches cannot be prevented due to congenital of nature or from underlying disease process; however, painful symptoms and future pathology from Flat Feet or Fallen Arches may be prevented by the following. Continue to wear your orthotics for work and exercise to provide stability and maintain function of your feet. Footwear. Continue to wear supportive shoes to maximise the function of your orthotic and prevent excessive movement of the joints in your feet.
After Care
Patients may go home the day of surgery or they may require an overnight hospital stay. The leg will be placed in a splint or cast and should be kept elevated for the first two weeks. At that point, sutures are removed. A new cast or a removable boot is then placed. It is important that patients do not put any weight on the corrected foot for six to eight weeks following the operation. Patients may begin bearing weight at eight weeks and usually progress to full weightbearing by 10 to 12 weeks. For some patients, weightbearing requires additional time. After 12 weeks, patients commonly can transition to wearing a shoe. Inserts and ankle braces are often used. Physical therapy may be recommended. There are complications that relate to surgery in general. These include the risks associated with anesthesia, infection, damage to nerves and blood vessels, and bleeding or blood clots. Complications following flatfoot surgery may include wound breakdown or nonunion (incomplete healing of the bones). These complications often can be prevented with proper wound care and rehabilitation. Occasionally, patients may notice some discomfort due to prominent hardware. Removal of hardware can be done at a later time if this is an issue. The overall complication rates for flatfoot surgery are low.

Fallen arches are a condition of the feet that can cause pain and discomfort. Normally, you should see an arch in the bottom of your foot. That arch is created by the tendons in your feet. The tendons pull, which forms the arch. Sometimes, the tendons do not pull as they should, which results in the condition of fallen arches. If you have fallen arches, your feet may look flat. You might also notice when you see your bare footprint that the arch is not visible in the print. It is fairly common for children to have flat feet, but the arch usually develops as it should as they get older. For adults, fallen arches can be quite painful and problematic.
Causes
The most common acquired flat foot in adults is due to Posterior Tibial Tendon Dysfunction. This develops with repetitive stress on the main supporting tendon of the arch over a long period of time. As the body ages, ligaments and muscles can weaken, leaving the job of supporting the arch all to this tendon. The tendon cannot hold all the weight for long, and it gradually gives out, leading to a progressively lower arch. This form of flat foot is often accompanied by pain radiating behind the ankle, consistent with the course of the posterior tibial tendon. Compounding matters is the fact that the human foot was not originally designed to withstand the types of terrain and forces it is subjected to today. Nowhere in nature do you see the flat hard surfaces that we so commonly walk on in present times. Walking on this type of surface continuously puts unnatural stress on the arch. The fact that the average American is overweight does not help the arch much either-obesity is a leading cause of flat feet as the arch collapses under the excessive bodyweight. Furthermore, the average life span has increased dramatically in the last century, meaning that not only does the arch deal with heavy weight on hard flat ground, but also must now do so for longer periods of time. These are all reasons to take extra care of our feet now in order to prevent problems later.
Symptoms
Many people have flat feet and notice no problems and require no treatment. But others may experience the following symptoms, Feet tire easily, painful or achy feet, especially in the areas of the arches and heels, the inside bottom of your feet become swollen, foot movement, such as standing on your toes, is difficult, back and leg pain, If you notice any of these symptoms, it's time for a trip to the doctor.
Diagnosis
It is important for people with foot pain to know if they have flat feet. The following tests can help you determine your arch type. When you get out of a swimming pool, look at your footprint on the concrete. The front of the foot will be joined to the heel by a strip. If your foot is flat, then the strip is the same width as the front of the foot, creating a footprint that looks like a stretched out pancake. With a normal arch, the strip is about half the width of the front of the foot. If you have a high arch, only a thin strip connects the front of the foot with the heel. Put your shoes on a flat table and view them at eye level from behind. See if the sole is worn evenly. A flat foot will cause more wear on the inside of the sole, especially in the heel area. The shoe will easily rock side to side. A flat foot will also cause the upper part of the shoe to lean inward over the sole. Both shoes should wear about the same way. If you have pain in one foot, you should make sure you don't have a fallen arch on that side. There are two good tests you can perform at home to detect this problem. Place your fingertips on a wall that you are directly facing and stand on your tiptoes on one foot. If you can't do it, a fallen arch may be the culprit. Stand with your feet parallel. Have someone stand in back of you and look at your feet from behind. You can also do it yourself if you stand with your back to a mirror. Normally, only the pinky toe is visible from behind. If one foot is flatter than the other, the 4th and sometimes the 3rd toe on that foot can also be seen.
What does it mean when you have flat feet?
Non Surgical Treatment
Ligaments hold up arches. Deformed ligaments will not return to their original shape, just as an overstretched rubber band remains elongated. Arch supports help restore more normal function. Not all orthotics are made alike. Sole Supports custom designed orthotics are unique in the way they are cast. Sole Supports compensate for the differences between each foot. They take into account your body weight and the degree of flexibility in your feet. Taking care of fallen arches can be key in dealing with unresolved or recurrent back pain.
Surgical Treatment

Surgery for flat feet is separated into three kinds: soft tissue procedures, bone cuts, and bone fusions. Depending on the severity of the flat foot, a person?s age, and whether or not the foot is stiff determines just how the foot can be fixed. In most cases a combination of procedures are performed. With flexible flat feet, surgery is geared at maintaining the motion of the foot and recreating the arch. Commonly this may involve tendon repairs along the inside of the foot to reinforce the main tendon that lifts the arch. When the bone collapse is significant, bone procedures are included to physically rebuild the arch, and realign the heel. The presence of bunions with flat feet is often contributing to the collapse and in most situations requires correction. With rigid flat feet, surgery is focused on restoring the shape of the foot through procedures that eliminate motion. In this case, motion does not exist pre-operatively, so realigning the foot is of utmost importance. The exception, are rigid flat feet due to tarsal coalition (fused segment of bone) in the back of the foot where freeing the blockage can restore function.
Prevention
Flat feet or Fallen Arches cannot be prevented due to congenital of nature or from underlying disease process; however, painful symptoms and future pathology from Flat Feet or Fallen Arches may be prevented by the following. Continue to wear your orthotics for work and exercise to provide stability and maintain function of your feet. Footwear. Continue to wear supportive shoes to maximise the function of your orthotic and prevent excessive movement of the joints in your feet.
After Care
Patients may go home the day of surgery or they may require an overnight hospital stay. The leg will be placed in a splint or cast and should be kept elevated for the first two weeks. At that point, sutures are removed. A new cast or a removable boot is then placed. It is important that patients do not put any weight on the corrected foot for six to eight weeks following the operation. Patients may begin bearing weight at eight weeks and usually progress to full weightbearing by 10 to 12 weeks. For some patients, weightbearing requires additional time. After 12 weeks, patients commonly can transition to wearing a shoe. Inserts and ankle braces are often used. Physical therapy may be recommended. There are complications that relate to surgery in general. These include the risks associated with anesthesia, infection, damage to nerves and blood vessels, and bleeding or blood clots. Complications following flatfoot surgery may include wound breakdown or nonunion (incomplete healing of the bones). These complications often can be prevented with proper wound care and rehabilitation. Occasionally, patients may notice some discomfort due to prominent hardware. Removal of hardware can be done at a later time if this is an issue. The overall complication rates for flatfoot surgery are low.
All You Might Want To Know About Heel Aches
Overview

Does it feel like you have a nail in your heel? After walking for a few minutes does the pain slowly disappear? Millions of people each year are faced with this type of pain. While there may be other causes, the most common is Plantar Fasciitis. Plantar Faciitis is an inflammation of the fibrous tissue, called the plantar fasciia, that runs along the bottom of your foot that connects the heel (calcaneus) to the toes (metatarsals). Treatment for this condition can take many forms including: stretching exercises, drugs, orthotics, injections, and in rare cases surgical procedures. Until now the treatment methods have addressed the active conscious periods only to be undone when a person goes to bed or sits in the easy chair relaxing.
Causes
While heel pain has many causes, it is usually the result of faulty biomechanics (abnormalities in the way we walk). This can place too much stress on the heel bone and the soft tissues attached to it. The stress may also result from injury, or a bruise incurred while walking, running or jumping on hard surfaces; wearing poorly constructed footwear; or being significantly overweight. Systemic diseases such as arthritis and diabetes can also contribute to heel pain. A common cause of heel pain is the heel spur, a bony growth under the heel bone. There are no visible features on the heel, but a deep painful spot can be found in or around the middle of the sole of the heel (see diagram). Approximately 10 per cent of the population may have heel spurs without any pain. Heel spurs result from strain on the muscles of the foot. This may result from biomechanical imbalance, a condition occurring in many people. Both heel pain and heel spurs are frequently associated with an inflammation of the long band of tissue that connects the heel and the ball of the foot. The inflammation of this arch area is called plantar fasciitis. The inflammation may be aggravated by shoes that lack appropriate support, especially in the arch area, and by the chronic irritation that sometimes accompanies an athletic lifestyle.Excessive rolling in of the feet when walking. An inflamed bursa (bursitis), a small, irritated sack of fluid at the back of the heel. A neuroma (a nerve growth). Other soft-tissue growths. Heel bumps or ?pump bumps?, a bone enlargement at the back of the heel bone. Bruises or stress fractures to the heel bone.
Symptoms
Usually when a patient comes in they?ll explain that they have severe pain in the heel. It?s usually worse during the first step in the morning when they get out of bed. Many people say if they walk for a period of time, it gets a little bit better. But if they sit down and get back up, the pain will come back and it?s one of those intermittent come and go types of pain. Heel pain patients will say it feels like a toothache in the heel area or even into the arch area. A lot of times it will get better with rest and then it will just come right back. So it?s one of those nuisance type things that just never goes away. The following are common signs of heel pain and plantar fasciitis. Pain that is worse first thing in the morning. Pain that develops after heavy activity or exercise. Pain that occurs when standing up after sitting for a long period of time. Severe, toothache type of pain in the bottom of the heel.
Diagnosis
A podiatrist (doctor who specializes in the evaluation and treatment of foot diseases) will carry out a physical examination, and ask pertinent questions about the pain. The doctor will also ask the patient how much walking and standing the patient does, what type of footwear is worn, and details of the his/her medical history. Often this is enough to make a diagnosis. Sometimes further diagnostic tests are needed, such as blood tests and imaging scans.
Non Surgical Treatment
Treatment of heel pain generally occurs in stages. At the earliest sign of heel pain, aggressive calf muscle stretching should be started. Additionally, taking an oral anti-inflammatory medication and over-the- counter arch supports or heel cushions may be beneficial. The next phase of treatment might consist of continued calf muscle stretching exercises, cortisone injections and orthopedic taping of the foot to support the arch. If this treatment fails, or if there is reoccurrence of the heel pain, then functional foot orthotics might be considered. A functional orthotic is a device that is prescribed and fitted by your foot doctor, which fits in normal shoes like an arch support. Unlike an arch support, however the orthotic corrects abnormal pronation of the subtalar joint. Thus orthotics address the cause of the heel pain - abnormal pronation of the foot. Pump bump, treatment is similar to the treatment of bursitis and heel spurs. In rare cases, the bony growth at the heel may need to be removed surgically. Heel bruises can be treated by applying an ice pack for the first few minutes after injury. Achilles tendonitis, this condition is treated conservatively with rest, NSAIDs and physical therapy. If a sprain, fracture or other injury has caused the trapped nerve, this underlying problem must be treated first. In rare cases, surgery may be done to release the trapped nerve.
Surgical Treatment
When a diagnosis of plantar fasciitis is made early, most patients respond to conservative treatment and don?t require surgical intervention. Often, when there is a secondary diagnosis contributing to your pain, such as an entrapped nerve, and you are non-responsive to conservative care, surgery may be considered. Dr. Talarico will discuss all options and which approach would be the most beneficial for your condition.
how to get rid of heel spurs
Prevention

You can try to avoid the things that cause heel pain to start avoid becoming overweight, where your job allows, minimise the shock to your feet from constant pounding on hard surfaces, reduce the shocks on your heel by choosing footwear with some padding or shock-absorbing material in the heel, if you have high-arched feet or flat feet a moulded insole in your shoe may reduce the stresses on your feet, if you have an injury to your ankle or foot, make sure you exercise afterwards to get back as much movement as possible to reduce the stresses on your foot and your heel in particular, If you start to get heel pain, doing the above things may enable the natural healing process to get underway and the pain to improve.

Does it feel like you have a nail in your heel? After walking for a few minutes does the pain slowly disappear? Millions of people each year are faced with this type of pain. While there may be other causes, the most common is Plantar Fasciitis. Plantar Faciitis is an inflammation of the fibrous tissue, called the plantar fasciia, that runs along the bottom of your foot that connects the heel (calcaneus) to the toes (metatarsals). Treatment for this condition can take many forms including: stretching exercises, drugs, orthotics, injections, and in rare cases surgical procedures. Until now the treatment methods have addressed the active conscious periods only to be undone when a person goes to bed or sits in the easy chair relaxing.
Causes
While heel pain has many causes, it is usually the result of faulty biomechanics (abnormalities in the way we walk). This can place too much stress on the heel bone and the soft tissues attached to it. The stress may also result from injury, or a bruise incurred while walking, running or jumping on hard surfaces; wearing poorly constructed footwear; or being significantly overweight. Systemic diseases such as arthritis and diabetes can also contribute to heel pain. A common cause of heel pain is the heel spur, a bony growth under the heel bone. There are no visible features on the heel, but a deep painful spot can be found in or around the middle of the sole of the heel (see diagram). Approximately 10 per cent of the population may have heel spurs without any pain. Heel spurs result from strain on the muscles of the foot. This may result from biomechanical imbalance, a condition occurring in many people. Both heel pain and heel spurs are frequently associated with an inflammation of the long band of tissue that connects the heel and the ball of the foot. The inflammation of this arch area is called plantar fasciitis. The inflammation may be aggravated by shoes that lack appropriate support, especially in the arch area, and by the chronic irritation that sometimes accompanies an athletic lifestyle.Excessive rolling in of the feet when walking. An inflamed bursa (bursitis), a small, irritated sack of fluid at the back of the heel. A neuroma (a nerve growth). Other soft-tissue growths. Heel bumps or ?pump bumps?, a bone enlargement at the back of the heel bone. Bruises or stress fractures to the heel bone.
Symptoms
Usually when a patient comes in they?ll explain that they have severe pain in the heel. It?s usually worse during the first step in the morning when they get out of bed. Many people say if they walk for a period of time, it gets a little bit better. But if they sit down and get back up, the pain will come back and it?s one of those intermittent come and go types of pain. Heel pain patients will say it feels like a toothache in the heel area or even into the arch area. A lot of times it will get better with rest and then it will just come right back. So it?s one of those nuisance type things that just never goes away. The following are common signs of heel pain and plantar fasciitis. Pain that is worse first thing in the morning. Pain that develops after heavy activity or exercise. Pain that occurs when standing up after sitting for a long period of time. Severe, toothache type of pain in the bottom of the heel.
Diagnosis
A podiatrist (doctor who specializes in the evaluation and treatment of foot diseases) will carry out a physical examination, and ask pertinent questions about the pain. The doctor will also ask the patient how much walking and standing the patient does, what type of footwear is worn, and details of the his/her medical history. Often this is enough to make a diagnosis. Sometimes further diagnostic tests are needed, such as blood tests and imaging scans.
Non Surgical Treatment
Treatment of heel pain generally occurs in stages. At the earliest sign of heel pain, aggressive calf muscle stretching should be started. Additionally, taking an oral anti-inflammatory medication and over-the- counter arch supports or heel cushions may be beneficial. The next phase of treatment might consist of continued calf muscle stretching exercises, cortisone injections and orthopedic taping of the foot to support the arch. If this treatment fails, or if there is reoccurrence of the heel pain, then functional foot orthotics might be considered. A functional orthotic is a device that is prescribed and fitted by your foot doctor, which fits in normal shoes like an arch support. Unlike an arch support, however the orthotic corrects abnormal pronation of the subtalar joint. Thus orthotics address the cause of the heel pain - abnormal pronation of the foot. Pump bump, treatment is similar to the treatment of bursitis and heel spurs. In rare cases, the bony growth at the heel may need to be removed surgically. Heel bruises can be treated by applying an ice pack for the first few minutes after injury. Achilles tendonitis, this condition is treated conservatively with rest, NSAIDs and physical therapy. If a sprain, fracture or other injury has caused the trapped nerve, this underlying problem must be treated first. In rare cases, surgery may be done to release the trapped nerve.
Surgical Treatment
When a diagnosis of plantar fasciitis is made early, most patients respond to conservative treatment and don?t require surgical intervention. Often, when there is a secondary diagnosis contributing to your pain, such as an entrapped nerve, and you are non-responsive to conservative care, surgery may be considered. Dr. Talarico will discuss all options and which approach would be the most beneficial for your condition.
how to get rid of heel spurs
Prevention

You can try to avoid the things that cause heel pain to start avoid becoming overweight, where your job allows, minimise the shock to your feet from constant pounding on hard surfaces, reduce the shocks on your heel by choosing footwear with some padding or shock-absorbing material in the heel, if you have high-arched feet or flat feet a moulded insole in your shoe may reduce the stresses on your feet, if you have an injury to your ankle or foot, make sure you exercise afterwards to get back as much movement as possible to reduce the stresses on your foot and your heel in particular, If you start to get heel pain, doing the above things may enable the natural healing process to get underway and the pain to improve.
Apparatus For Leg Length Discrepancy Measurement
Overview
Limb-length discrepancies or differences are conditions that result in limbs that are unequal in length or that exhibit other anomalies. The conditions occur when bones or joints in the arms or legs are abnormal or become damaged. Providers might refer to these conditions as limb-length discrepancies, limb differences or limb-length conditions.
Causes
From an anatomical stand point, the LLD could have been from hereditary, broken bones, diseases and joint replacements. Functional LLD can be from over pronating, knee deformities, tight calves and hamstrings, weak IT band, curvature in the spine and many other such muscular/skeletal issues.
Symptoms
The most common symptom of all forms of LLD is chronic backache. In structural LLD the sufferer may also experience arthritis within the knee and hip are, flank pain, plantar fasciitis and metatarsalgia all on the side that is longer. Functional LLD sufferers will see similar conditions on the shorter side.
Diagnosis
A qualified musculoskeletal expert will first take a medical history and conduct a physical exam. Other tests may include X-rays, MRI, or CT scan to diagnose the root cause.
Non Surgical Treatment
The object of treatment for leg length discrepancy is to level the pelvis and equalize the length of the two limbs. Inequalities of 2-2.5 centimeters can be handled with the following. Heel lifts/ adjustable heel lifts can be used inside a shoe where shoes have a full heel counter. Heel lifts may be added to the heel on the outside of the shoe along with an internal heel lift. Full platforms along the forefoot and rearfoot area of a shoe can be added. There are many different adjustable heel lifts available on the market. For treatment of a leg length discrepancy, consult your physician. They may refer you to a Physiotherapist or Chiropractor for determination of the type of LLD. A Certified Pedorthist (Canada) will treat a structural leg length discrepancy with a heel lift or in larger discrepancies a footwear modification.

how to grow taller at 14
Surgical Treatment
In growing children, legs can be made equal or nearly equal in length with a relatively simple surgical procedure. This procedure slows down the growth of the longer leg at one or two growth sites. Your physician can tell you how much equalization can be gained by this procedure. The procedure is performed under X-ray control through very small incisions in the knee area. This procedure will not cause an immediate correction in length. Instead, the limb length discrepancy will gradually decrease as the opposite extremity continues to grow and "catch up." Timing of the procedure is critical. The goal is to reach equal leg length by the time growth normally ends. This is usually in the mid-to-late teenage years. Disadvantages of this option include the possibility of slight over-correction or under-correction of the limb length discrepancy. In addition, the patient's adult height will be less than if the shorter leg had been lengthened. Correction of significant limb length discrepancy by this method may make a patient's body look slightly disproportionate because of the shorter leg. In some cases the longer leg can be shortened, but a major shortening may weaken the muscles of the leg. In the thighbone (femur), a maximum of 3 inches can be shortened. In the shinbone, a maximum of 2 inches can be shortened.
Limb-length discrepancies or differences are conditions that result in limbs that are unequal in length or that exhibit other anomalies. The conditions occur when bones or joints in the arms or legs are abnormal or become damaged. Providers might refer to these conditions as limb-length discrepancies, limb differences or limb-length conditions.

Causes
From an anatomical stand point, the LLD could have been from hereditary, broken bones, diseases and joint replacements. Functional LLD can be from over pronating, knee deformities, tight calves and hamstrings, weak IT band, curvature in the spine and many other such muscular/skeletal issues.
Symptoms
The most common symptom of all forms of LLD is chronic backache. In structural LLD the sufferer may also experience arthritis within the knee and hip are, flank pain, plantar fasciitis and metatarsalgia all on the side that is longer. Functional LLD sufferers will see similar conditions on the shorter side.
Diagnosis
A qualified musculoskeletal expert will first take a medical history and conduct a physical exam. Other tests may include X-rays, MRI, or CT scan to diagnose the root cause.
Non Surgical Treatment
The object of treatment for leg length discrepancy is to level the pelvis and equalize the length of the two limbs. Inequalities of 2-2.5 centimeters can be handled with the following. Heel lifts/ adjustable heel lifts can be used inside a shoe where shoes have a full heel counter. Heel lifts may be added to the heel on the outside of the shoe along with an internal heel lift. Full platforms along the forefoot and rearfoot area of a shoe can be added. There are many different adjustable heel lifts available on the market. For treatment of a leg length discrepancy, consult your physician. They may refer you to a Physiotherapist or Chiropractor for determination of the type of LLD. A Certified Pedorthist (Canada) will treat a structural leg length discrepancy with a heel lift or in larger discrepancies a footwear modification.

how to grow taller at 14
Surgical Treatment
In growing children, legs can be made equal or nearly equal in length with a relatively simple surgical procedure. This procedure slows down the growth of the longer leg at one or two growth sites. Your physician can tell you how much equalization can be gained by this procedure. The procedure is performed under X-ray control through very small incisions in the knee area. This procedure will not cause an immediate correction in length. Instead, the limb length discrepancy will gradually decrease as the opposite extremity continues to grow and "catch up." Timing of the procedure is critical. The goal is to reach equal leg length by the time growth normally ends. This is usually in the mid-to-late teenage years. Disadvantages of this option include the possibility of slight over-correction or under-correction of the limb length discrepancy. In addition, the patient's adult height will be less than if the shorter leg had been lengthened. Correction of significant limb length discrepancy by this method may make a patient's body look slightly disproportionate because of the shorter leg. In some cases the longer leg can be shortened, but a major shortening may weaken the muscles of the leg. In the thighbone (femur), a maximum of 3 inches can be shortened. In the shinbone, a maximum of 2 inches can be shortened.
Leg Length Discrepancy Women
Overview
Surgery to shorten the longer leg. This is less involved than lengthening the shorter leg. Shortening may be done in one of two ways. Closing the growth plate of the long leg 2-3 years before growth ends (around age 11-13), letting the short leg catch up. This procedure is called an epiphysiodesis. Taking some bone from the longer leg once growth is complete to even out leg lengths. Surgery to lengthen the shorter leg. This surgery is more involved than surgery to shorten a leg. During this surgery, cuts are made in the leg bone. An external metal frame and bar are attached to the leg bone. This frame and bar slowly pull on the leg bone, lengthening it. The frame and bar must be worn constantly for months to years. When the frame and bar are removed, a leg cast is required for several months. This surgery requires careful and continued follow-up with the surgeon to be sure that healing is going well.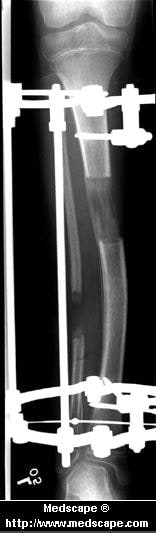
Causes
Leg length discrepancies can be caused by: hip and knee replacements, lower limb injuries, bone diseases, neuromuscular issues and congenital problems. Although discrepancies of 2 cm or less are most common, discrepancies can be greater than 6 cm. People who have LLD tend to make up for the difference by over bending their longer leg or standing on the toes of their shorter leg. This compensation leads to an inefficient, up and down gait, which is quite tiring and over time can result in posture problems as well as pain in the back, hips, knees and ankles.
Symptoms
Back pain along with pain in the foot, knee, leg and hip on one side of the body are the main complaints. There may also be limping or head bop down on the short side or uneven arm swinging. The knee bend, hip or shoulder may be down on one side, and there may be uneven wear to the soles of shoes (usually more on the longer side).
Diagnosis
Leg length discrepancy may be diagnosed during infancy or later in childhood, depending on the cause. Conditions such as hemihypertrophy or hemiatrophy are often diagnosed following standard newborn or infant examinations by a pediatrician, or anatomical asymmetries may be noticed by a child's parents. For young children with hemihypertophy as the cause of their LLD, it is important that they receive an abdominal ultrasound of the kidneys to insure that Wilm's tumor, which can lead to hypertrophy in the leg on the same side, is not present. In older children, LLD is frequently first suspected due to the emergence of a progressive limp, warranting a referral to a pediatric orthopaedic surgeon. The standard workup for LLD is a thorough physical examination, including a series of measurements of the different portions of the lower extremities with the child in various positions, such as sitting and standing. The orthopaedic surgeon will observe the child while walking and performing other simple movements or tasks, such as stepping onto a block. In addition, a number of x-rays of the legs will be taken, so as to make a definitive diagnosis and to assist with identification of the possible etiology (cause) of LLD. Orthopaedic surgeons will compare x-rays of the two legs to the child's age, so as to assess his/her skeletal age and to obtain a baseline for the possibility of excessive growth rate as a cause. A growth chart, which compares leg length to skeletal age, is a simple but essential tool used over time to track the progress of the condition, both before and after treatment. Occasionally, a CT scan or MRI is required to further investigate suspected causes or to get more sophisticated radiological pictures of bone or soft tissue.
Non Surgical Treatment
Treatments for limb-length discrepancies and differences vary, depending on the cause and severity of the condition. At Gillette, our orthopedic surgeons are experts in typical and atypical growth and development. Our expertise lets us plan treatments that offer a lifetime of benefits. Treatments might include monitoring growth and development, providing noninvasive treatments or therapy, and providing a combination of orthopedic surgical procedures. To date, alternative treatments (such as chiropractic care or physical therapy) have not measurably altered the progression of or improved limb-length conditions. However, children often have physical or occupational therapy to address related conditions, such as muscle weakness or inflexibility, or to speed recovery following a surgical procedure. In cases where surgical treatment isn?t necessary, our orthopedists may monitor patients and plan noninvasive treatments, such as, occupational therapy, orthoses (braces) and shoe inserts, physical therapy, prostheses (artificial limbs).

how to increase height naturally after 18
Surgical Treatment
Leg shortening is employed when LLD is severe and when a patient has already reached skeletal maturity. The actual surgery is called an osteotomy , which entails the removal of a small section of bone in the tibia (shinbone) and sometimes the fibula as well, resulting in the loss of around an inch in total height. Leg lengthening is a difficult third option that has traditionally had a high complication rate. Recently, results have improved somewhat with the emergence of a technique known as callotasis , in which only the outer portion of the bone (the cortex ) is cut, (i.e. a corticotomy ). This allows the bone to be more easily lengthened by an external fixation device that is attached to either side of the cut bone with pins through the skin. The ?ex-fix,' as it is sometimes called, is gradually adjusted by an orthopaedic surgeon, and healing can occur at the same time that the leg is being distracted , or lengthened over time. Unlike epiphysiodesis, leg lengthening procedures can be performed at almost any skeletal or chronological age.
Surgery to shorten the longer leg. This is less involved than lengthening the shorter leg. Shortening may be done in one of two ways. Closing the growth plate of the long leg 2-3 years before growth ends (around age 11-13), letting the short leg catch up. This procedure is called an epiphysiodesis. Taking some bone from the longer leg once growth is complete to even out leg lengths. Surgery to lengthen the shorter leg. This surgery is more involved than surgery to shorten a leg. During this surgery, cuts are made in the leg bone. An external metal frame and bar are attached to the leg bone. This frame and bar slowly pull on the leg bone, lengthening it. The frame and bar must be worn constantly for months to years. When the frame and bar are removed, a leg cast is required for several months. This surgery requires careful and continued follow-up with the surgeon to be sure that healing is going well.

Causes
Leg length discrepancies can be caused by: hip and knee replacements, lower limb injuries, bone diseases, neuromuscular issues and congenital problems. Although discrepancies of 2 cm or less are most common, discrepancies can be greater than 6 cm. People who have LLD tend to make up for the difference by over bending their longer leg or standing on the toes of their shorter leg. This compensation leads to an inefficient, up and down gait, which is quite tiring and over time can result in posture problems as well as pain in the back, hips, knees and ankles.
Symptoms
Back pain along with pain in the foot, knee, leg and hip on one side of the body are the main complaints. There may also be limping or head bop down on the short side or uneven arm swinging. The knee bend, hip or shoulder may be down on one side, and there may be uneven wear to the soles of shoes (usually more on the longer side).
Diagnosis
Leg length discrepancy may be diagnosed during infancy or later in childhood, depending on the cause. Conditions such as hemihypertrophy or hemiatrophy are often diagnosed following standard newborn or infant examinations by a pediatrician, or anatomical asymmetries may be noticed by a child's parents. For young children with hemihypertophy as the cause of their LLD, it is important that they receive an abdominal ultrasound of the kidneys to insure that Wilm's tumor, which can lead to hypertrophy in the leg on the same side, is not present. In older children, LLD is frequently first suspected due to the emergence of a progressive limp, warranting a referral to a pediatric orthopaedic surgeon. The standard workup for LLD is a thorough physical examination, including a series of measurements of the different portions of the lower extremities with the child in various positions, such as sitting and standing. The orthopaedic surgeon will observe the child while walking and performing other simple movements or tasks, such as stepping onto a block. In addition, a number of x-rays of the legs will be taken, so as to make a definitive diagnosis and to assist with identification of the possible etiology (cause) of LLD. Orthopaedic surgeons will compare x-rays of the two legs to the child's age, so as to assess his/her skeletal age and to obtain a baseline for the possibility of excessive growth rate as a cause. A growth chart, which compares leg length to skeletal age, is a simple but essential tool used over time to track the progress of the condition, both before and after treatment. Occasionally, a CT scan or MRI is required to further investigate suspected causes or to get more sophisticated radiological pictures of bone or soft tissue.
Non Surgical Treatment
Treatments for limb-length discrepancies and differences vary, depending on the cause and severity of the condition. At Gillette, our orthopedic surgeons are experts in typical and atypical growth and development. Our expertise lets us plan treatments that offer a lifetime of benefits. Treatments might include monitoring growth and development, providing noninvasive treatments or therapy, and providing a combination of orthopedic surgical procedures. To date, alternative treatments (such as chiropractic care or physical therapy) have not measurably altered the progression of or improved limb-length conditions. However, children often have physical or occupational therapy to address related conditions, such as muscle weakness or inflexibility, or to speed recovery following a surgical procedure. In cases where surgical treatment isn?t necessary, our orthopedists may monitor patients and plan noninvasive treatments, such as, occupational therapy, orthoses (braces) and shoe inserts, physical therapy, prostheses (artificial limbs).

how to increase height naturally after 18
Surgical Treatment
Leg shortening is employed when LLD is severe and when a patient has already reached skeletal maturity. The actual surgery is called an osteotomy , which entails the removal of a small section of bone in the tibia (shinbone) and sometimes the fibula as well, resulting in the loss of around an inch in total height. Leg lengthening is a difficult third option that has traditionally had a high complication rate. Recently, results have improved somewhat with the emergence of a technique known as callotasis , in which only the outer portion of the bone (the cortex ) is cut, (i.e. a corticotomy ). This allows the bone to be more easily lengthened by an external fixation device that is attached to either side of the cut bone with pins through the skin. The ?ex-fix,' as it is sometimes called, is gradually adjusted by an orthopaedic surgeon, and healing can occur at the same time that the leg is being distracted , or lengthened over time. Unlike epiphysiodesis, leg lengthening procedures can be performed at almost any skeletal or chronological age.
Mortons Neuroma Prevention
Overview
 A neuroma develops when a nerve is compressed, injured or pinched, causing swelling and pain. A neuroma in the area between the third and fourth toes, or between the second and third toes, is known as a Morton?s neuroma. Morton?s neuroma causes sharp, burning pain and numbness in the toes and foot. You may feel like you?ve stepped on a tiny hot coal and can?t get rid of it. At the same time, you?ll have the disconcerting experience of not being able to feel your toes. Sometimes the nerve tissue becomes so thickened you can feel or see a lump.
A neuroma develops when a nerve is compressed, injured or pinched, causing swelling and pain. A neuroma in the area between the third and fourth toes, or between the second and third toes, is known as a Morton?s neuroma. Morton?s neuroma causes sharp, burning pain and numbness in the toes and foot. You may feel like you?ve stepped on a tiny hot coal and can?t get rid of it. At the same time, you?ll have the disconcerting experience of not being able to feel your toes. Sometimes the nerve tissue becomes so thickened you can feel or see a lump.
Causes
When a nerve is pinched between bones, the result is swelling of the nerve. It is this swelling which is referred to as a Neuroma. When the condition occurs in the foot, it is known as a Morton?s Neuroma. Morton?s Neuroma is technically not a tumor. Rather, it is a thickening of the tissue that surrounds the digital nerves leading to the toes. These nerves allow for physical sensation on the skin of the toes. The region of inflammation is found where the digital nerve passes under the ligament connecting the toe bones (metatarsals) in the forefoot. Morton?s Neuroma commonly develops between the third and fourth toes, generally as a result of ongoing irritation, trauma or excessive pressure. In some cases, the second and third toes are involved. Morton?s Neuroma is confined to one foot in most cases, though it can occur in both, particularly in athletes such as runners.
Symptoms
Patients will feel pain that worsens with walking, particularly when walking in shoes with thin soles or high heels. Also, anything that squeezes the metatarsal heads together may aggravate symptoms, such as narrow shoes. A patient may feel the need to remove the shoe and rub the foot to soothe the pain.
Diagnosis
Podiatrists conduct a physical examination and may order imaging tests, such as x-ray or MRI scan to diagnose Morton's neuroma. Conservative treatment options include custom-fitted orthotics, medication, and/or alcohol injections designed to harden the nerve. However, most patients with Morton's neuroma need minor surgery.
Non Surgical Treatment
Simple treatments may be all that are needed for some people with a Morton's neuroma. They include the following. Footwear adjustments including avoidance of high-heeled and narrow shoes and having special orthotic pads and devices fitted into your shoes. Calf-stretching exercises may also be taught to help relieve the pressure on your foot. Steroid or local anaesthetic injections (or a combination of both) into the affected area of the foot may be needed if the simple footwear changes do not fully relieve symptoms. However, the footwear modification measures should still be continued. Sclerosant injections involve the injection of alcohol and local anaesthetic into the affected nerve under the guidance of an ultrasound scan. Some studies have shown this to be as effective as surgery.
Surgical Treatment
Surgery is occasionally required when the conservative treatment is not able to relieve your symptoms, particularly if you have had pain for more than 6 months. 80% of patients who require surgery report good results, with 71% of people becoming pain-free.
 A neuroma develops when a nerve is compressed, injured or pinched, causing swelling and pain. A neuroma in the area between the third and fourth toes, or between the second and third toes, is known as a Morton?s neuroma. Morton?s neuroma causes sharp, burning pain and numbness in the toes and foot. You may feel like you?ve stepped on a tiny hot coal and can?t get rid of it. At the same time, you?ll have the disconcerting experience of not being able to feel your toes. Sometimes the nerve tissue becomes so thickened you can feel or see a lump.
A neuroma develops when a nerve is compressed, injured or pinched, causing swelling and pain. A neuroma in the area between the third and fourth toes, or between the second and third toes, is known as a Morton?s neuroma. Morton?s neuroma causes sharp, burning pain and numbness in the toes and foot. You may feel like you?ve stepped on a tiny hot coal and can?t get rid of it. At the same time, you?ll have the disconcerting experience of not being able to feel your toes. Sometimes the nerve tissue becomes so thickened you can feel or see a lump.Causes
When a nerve is pinched between bones, the result is swelling of the nerve. It is this swelling which is referred to as a Neuroma. When the condition occurs in the foot, it is known as a Morton?s Neuroma. Morton?s Neuroma is technically not a tumor. Rather, it is a thickening of the tissue that surrounds the digital nerves leading to the toes. These nerves allow for physical sensation on the skin of the toes. The region of inflammation is found where the digital nerve passes under the ligament connecting the toe bones (metatarsals) in the forefoot. Morton?s Neuroma commonly develops between the third and fourth toes, generally as a result of ongoing irritation, trauma or excessive pressure. In some cases, the second and third toes are involved. Morton?s Neuroma is confined to one foot in most cases, though it can occur in both, particularly in athletes such as runners.
Symptoms
Patients will feel pain that worsens with walking, particularly when walking in shoes with thin soles or high heels. Also, anything that squeezes the metatarsal heads together may aggravate symptoms, such as narrow shoes. A patient may feel the need to remove the shoe and rub the foot to soothe the pain.
Diagnosis
Podiatrists conduct a physical examination and may order imaging tests, such as x-ray or MRI scan to diagnose Morton's neuroma. Conservative treatment options include custom-fitted orthotics, medication, and/or alcohol injections designed to harden the nerve. However, most patients with Morton's neuroma need minor surgery.
Non Surgical Treatment
Simple treatments may be all that are needed for some people with a Morton's neuroma. They include the following. Footwear adjustments including avoidance of high-heeled and narrow shoes and having special orthotic pads and devices fitted into your shoes. Calf-stretching exercises may also be taught to help relieve the pressure on your foot. Steroid or local anaesthetic injections (or a combination of both) into the affected area of the foot may be needed if the simple footwear changes do not fully relieve symptoms. However, the footwear modification measures should still be continued. Sclerosant injections involve the injection of alcohol and local anaesthetic into the affected nerve under the guidance of an ultrasound scan. Some studies have shown this to be as effective as surgery.

Surgical Treatment
Surgery is occasionally required when the conservative treatment is not able to relieve your symptoms, particularly if you have had pain for more than 6 months. 80% of patients who require surgery report good results, with 71% of people becoming pain-free.
The Ideal Solution To Leg Length Imbalances Are Shoe Lifts
There are actually two different types of leg length discrepancies, congenital and acquired. Congenital means you are born with it. One leg is structurally shorter in comparison to the other. As a result of developmental stages of aging, the human brain picks up on the walking pattern and recognizes some variance. The entire body typically adapts by tilting one shoulder to the "short" side. A difference of less than a quarter inch is not very abnormal, require Shoe Lifts to compensate and mostly doesn't have a profound effect over a lifetime.

Leg length inequality goes typically undiagnosed on a daily basis, however this issue is easily corrected, and can reduce quite a few incidents of back discomfort.
Treatment for leg length inequality usually involves Shoe Lifts . Most are economical, normally priced at less than twenty dollars, in comparison to a custom orthotic of $200 if not more. When the amount of leg length inequality begins to exceed half an inch, a whole sole lift is generally the better choice than a heel lift. This prevents the foot from being unnecessarily stressed in an abnormal position.
Chronic back pain is easily the most prevalent condition affecting people today. Over 80 million people have problems with back pain at some stage in their life. It's a problem which costs businesses millions each year as a result of time lost and production. Fresh and superior treatment solutions are always sought after in the hope of reducing the economical influence this issue causes.

Men and women from all corners of the earth suffer the pain of foot ache due to leg length discrepancy. In these situations Shoe Lifts are usually of beneficial. The lifts are capable of easing any discomfort and pain in the feet. Shoe Lifts are recommended by numerous specialist orthopaedic orthopedists.
So that they can support the body in a well-balanced fashion, feet have a critical role to play. Despite that, it is sometimes the most overlooked area in the human body. Some people have flat-feet meaning there may be unequal force exerted on the feet. This will cause other areas of the body such as knees, ankles and backs to be affected too. Shoe Lifts ensure that proper posture and balance are restored.

Leg length inequality goes typically undiagnosed on a daily basis, however this issue is easily corrected, and can reduce quite a few incidents of back discomfort.
Treatment for leg length inequality usually involves Shoe Lifts . Most are economical, normally priced at less than twenty dollars, in comparison to a custom orthotic of $200 if not more. When the amount of leg length inequality begins to exceed half an inch, a whole sole lift is generally the better choice than a heel lift. This prevents the foot from being unnecessarily stressed in an abnormal position.
Chronic back pain is easily the most prevalent condition affecting people today. Over 80 million people have problems with back pain at some stage in their life. It's a problem which costs businesses millions each year as a result of time lost and production. Fresh and superior treatment solutions are always sought after in the hope of reducing the economical influence this issue causes.

Men and women from all corners of the earth suffer the pain of foot ache due to leg length discrepancy. In these situations Shoe Lifts are usually of beneficial. The lifts are capable of easing any discomfort and pain in the feet. Shoe Lifts are recommended by numerous specialist orthopaedic orthopedists.
So that they can support the body in a well-balanced fashion, feet have a critical role to play. Despite that, it is sometimes the most overlooked area in the human body. Some people have flat-feet meaning there may be unequal force exerted on the feet. This will cause other areas of the body such as knees, ankles and backs to be affected too. Shoe Lifts ensure that proper posture and balance are restored.
Do I Have Posterior Calcaneal Spur

Overview
In the setting of plantar fasciitis, heel spurs are most often seen in middle-aged men and women, but can be found in all age groups. The heel spur itself is not thought to be the primary cause of pain, rather inflammation and irritation of the plantar fascia is thought to be the primary problem. A heel spur diagnosis is made when an x-ray shows a hook of bone protruding from the bottom of the foot at the point where the plantar fascia is attached to the heel bone.
Causes
Though this syndrome is most common in individuals 40 years or older, it can occur at any age. The following factors increase the likelihood of heel spur development. An uneven gait which applies too much pressure to certain areas of the foot. Being overweight. Wearing worn shoes or ill-fitting footwear. Job conditions that require long periods spent standing or lifting heavy objects. The normal aging process which results in a decrease in ligament elasticity.

Symptoms
The following symptoms are typical of heel spur. Stabbing pain when treading on the area affected. Dull, irregularly occurring pains in the heel area also without exerting pressure (e.g. in a reclining position) Pain when taking the first steps in the morning (after lying or sitting down for an extended period, especially in the morning) Occasional swelling in the ankle area. For the lower heel spur, extreme sensitivity at the tendon attachment (laterally in the lower heel area) For the upper heel spur, extreme pressure sensitivity of the Achilles tendon, primarily at approximately ankle height.
Diagnosis
Heel spurs and plantar fasciitis is usually diagnosed by your physiotherapist or sports doctor based on your symptoms, history and clinical examination. After confirming your heel spur or plantar fasciitis they will investigate WHY you are likely to be predisposed to heel spurs and develop a treatment plan to decrease your chance of future bouts. X-rays will show calcification or bone within the plantar fascia or at its insertion into the calcaneus. This is known as a calcaneal or heel spur. Ultrasound scans and MRI are used to identify any plantar fasciitis tears, inflammation or calcification. Pathology tests may identify spondyloarthritis, which can cause symptoms similar to plantar fasciitis.
Non Surgical Treatment
There are many temporary solutions to resolve the pain associated with irritation to the plantar ligaments. Common recommendations are ice and anti-inflammatory medications or even cortisone injections, however none of these solve the fundamental problem. To permanently resolve heel spurs you need to support and restrict the movement of the plantar ligaments. Flexible shoes will aggravate and often contribute to heel spurs. We recommend a RIGID orthotic that extends from the metatarsal heads to the heel to resolve heel spurs.
Surgical Treatment
When chronic heel pain fails to respond to conservative treatment, surgical treatment may be necessary. Heel surgery can provide pain relief and restore mobility. The type of procedure used is based on examination and usually consists of releasing the excessive tightness of the plantar fascia, called a plantar fascia release. The procedure may also include removal of heel spurs.
Prevention
In order to prevent heel spurs, it?s important that you pay attention to the physical activities you engage in. Running or jogging on hard surfaces, such as cement or blacktop, is typical for competitive runners, but doing this for too long without breaks can lead to heel spurs and foot pain. Likewise, the shoes you wear can make a big difference in whether or not you develop heel spurs. Have your shoes and feet checked regularly by our Dallas podiatrist to ensure that you are wearing the proper equipment for the activities. Regular checkups with a foot and ankle specialist can help avoid the development of heel spurs.